Previously, a significant association between obstructive sleep apnea (OSA) and severe COVID-19 acute infection was established. New research suggests that OSA may also impact recovery and health beyond acute infection.
A recent study supported by the National Institutes of Health found that among people who have had COVID-19, adults with obstructive sleep apnea are more likely to experience long-term symptoms suggestive of long COVID than those without OSA, based on the electronic health record data of more than 2.2 million Americans with COVID-19.
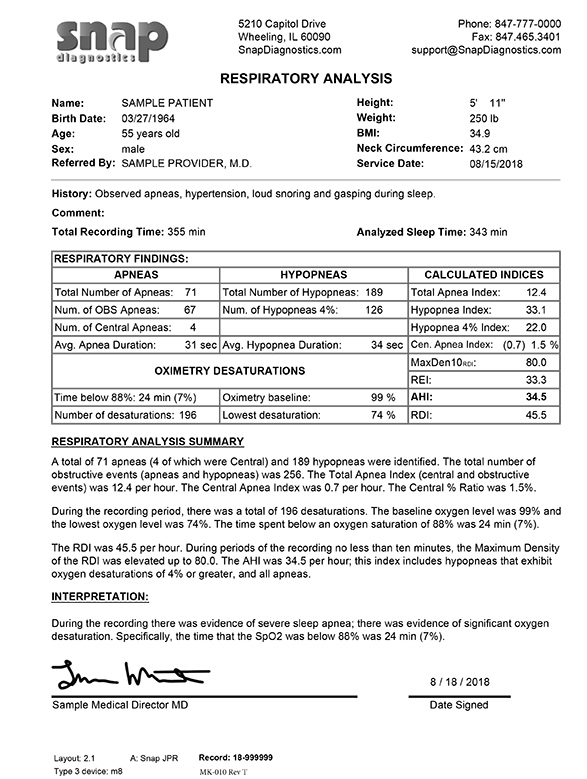
Identifying Sleep Apnea:
The most common symptoms of sleep apnea include snoring, gasping, or choking during sleep, morning headaches, and daytime sleepiness. Risk factors associated with sleep apnea include high body mass index (BMI), obesity, older age (>40 years old), and certain anatomical features such as enlarged tonsils or upper airway abnormalities. Use of tobacco, alcohol, and certain sedative and pain medications may increase apnea severity.
Sleep apnea is a common comorbidity in patients with heart disease, stroke, high blood pressure, GI reflux disease, high cholesterol, and type II diabetes.



Recent Comments